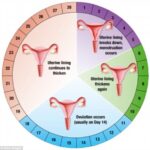
Eshre definition:
At least two of the following three features must be presentTwo episodes of POR after maximal stimulation are sufficient to define a patient as poor responder in the absence of advanced maternal age or abnormal ORT
Other Definitions
–Three or fewer recruited follicles or collected oocytes and a serum estradiol concentration lower than 300 pg/mL (if one follicle) or 500 pg/mL (if 2 or 3 follicles) at the time of hCG administration.
–Patients undergoing treatment with ICSI, IVF, or TESE/ ICSI from whom fewer than 5, 6, or 8 oocytes are retrieved.
–be those patients who fail to develop more than three preovulatory follicles after using more than 300 IU of daily FSH or when it requires more than 3000 IU FSH to recruit less than four follicles.
Incidence of poor responder:
It is not very uncommon. Incidence is between 9-24 %. This incidence has wide range , as it depends on individual IVF centre what they define as poor responder. Data from the ASRM registry showed that 14.1% of initial cycles were cancelled; at least 50% of these were poor responders
CLASSIFICATION OF POOR RESPONDER:
Categorized into two subgroups those in whom poor ovarian response has been observed in previous stimulated cycles those in whom poor ovarian response is expected based on ovarian reserve tests or other factors such as age, ovarian surgery,
Etiologies of poor ovarian Response:
Poor ovarian reserve is correlated with advanced maternal age but it can also occur in young female with endometriosis, prior ovarian surgery, pelvic adhesions and smoking. However, following conditions are also associated with unknown etiologies in young female.
what can be modified for poor responders ?
Gonadotropins
Standard dose of gonadotropins is 225IU to 300 IU. Dose are increased in these patients upto 450 IU AND sometimes to 6OOIU. But, different studies showed that even if we increase the dose of FSH, it does not result in better pregnancy outcomes. Because oocyte retrieval depends on number of basline follicles before stimulation.
GnRH
Long protocols with GnRH agoinst from luteal phase were used previously for lower cycle cancellation and better oocyte retrieval but now it is said in poor responder it causes more suppression ovarian suppression and that could lead to a reduced or absent follicular response.